Metatarsal and Phalangeal (Forefoot) Fractures
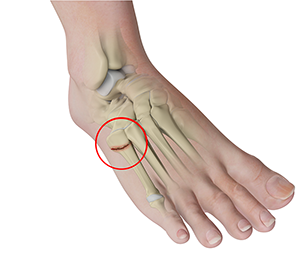
Forefoot Fractures
The forefoot is the anterior or front portion of the foot that functions in weight-bearing and maintaining balance while standing, walking or running. It is formed by 5 metatarsal bones, 14 phalange bones, and various soft tissues. A forefoot fracture is a crack or breaks in any of these bones. In some cases, the broken bone can protrude through the skin. These are called open fractures.
Causes
Stress fractures of the metatarsals are common especially with athletes. The 2nd metatarsal (MT) and the 4th MT are particularly vulnerable. They occur usually with an increase in intensity or duration of training. Metabolic deficiencies are also common especially with a lack of Vitamin D as well as Calcium.
Traumatic fractures occur when there is a direct impact of your foot on a hard surface. Stress fractures are tiny hairline cracks in the bone, most often caused due to repeated stress. Stress fractures are common in dancers, runners, and athletes.
Symptoms
The common symptoms of forefoot fracture include:
- Pain
- Bruising
- Swelling
- Inability to walk
Diagnosis
Your doctor will physically examine the forefoot and assess the injury. An X-ray will be ordered to examine the fracture more closely.
Treatment
The treatment options include:
- Medications: Prescribed pain medications may be given to manage pain.
- Rest: Adequate rest can heal a traumatic fracture.
- Splinting: Splints may be applied to keep the toe in a fixed position.
- Rigid shoe: A stiff-soled shoe may be recommended to protect the toe and position it correctly.
- Buddy-taping: The fractured toe is taped to the adjacent toe with a gauze pad between the toes.
- Cross training: to off-load affected MT
- Metabolic Balance: with Vitamin D & Calcium
- Bone Stimulator: at home regiment
- Shockwave Therapy Treatment: 1x/week for 3 weeks in office
Surgery is recommended if you do not respond to non-surgical treatment options. The surgery is performed under local anesthesia. Your surgeon realigns the fractured bones using pins or screws to hold the bones together in place until they heal completely. Follow-up X-rays may be ordered to monitor complete healing which may take about 6-8 weeks.
Dr. Kennedy's Articles
Resolution of metatarsalgia following oblique osteotomy