Hallux Valgus Surgery: Bunions
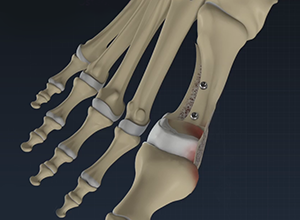
Bunions are a common source of pain in the forefoot for both women and men. They may be associated with other conditions such as flat foot where the forefoot over pronates, or may be congenital in origin. In times past, patients were advised to wait until the deformity was severe and the pain was intolerable before considering surgery. Now we advocate early intervention so that the joint cartilage can be saved.
Diagnosis
Your doctor may order X-rays to help determine the extent of damage and deformity of the toe joints.
Surgical Treatment of Hallux Valgus
Hallux valgus is a condition that is treated with excellent outcomes using minimally invasive techniques. There are many surgical options to treat a bunion but the common goal is to realign the joint, correct the deformity, and to relieve pain and discomfort. Your surgeon will discuss the different options available to you and a plan specific to your foot will be agreed upon before your surgery.
Osteotomy
It is a common type of bunion surgery that involves surgical cutting and realignment of the toe joint. The orthopedic surgeon selects the appropriate surgical procedure based on the patient's presentation. There are 3 types of osteotomies, namely akin osteotomy, chevron osteotomy, and scarf osteotomy.
1. SCARF Osteotomy
The Scarf osteotomy has been used extensively for 40 years and we have one of the largest published series in the USA on this procedure with excellent outcomes. Scarf osteotomy is usually recommended for moderate to severe bunion deformities. Your surgeon will make an incision along your big toe and open up the joint capsule to expose the bump. The bump on your big toe is then removed using a bone saw. Your first metatarsal bone is then cut in a Z shape and realigned to correct the deformity. Your surgeon will fix the cut bone with pins or screws. The joint capsule and surgical wounds are then re-approximated using dissolvable sutures keeping your toe in a straight position.
A rotational scarf osteotomy decreases troughing when treating hallux valgus
2. Akin Osteotomy
Your surgeon will make an incision along your big toe. The joint capsule is then opened, and the bunion is removed using a surgical saw. Your surgeon will then remove a wedge of bone from your big toe. Your toe is then brought back to its normal anatomical position and held together with surgical staples. The mobility of your big toe is examined, and the capsule and wound are re-approximated with sutures.
3. Chevron Osteotomy
A chevron osteotomy is usually recommended for mild to moderate bunion deformities. During this procedure, your surgeon will make an incision over your big toe. The joint capsule is opened, and the bunion is removed using a surgical saw. A V-shaped cut is made on the metatarsal bone of your big toe, and the bones are moved to bring your toe into its normal anatomical position. Screws or pins are used to hold the bones in their new position until healing occurs. The mobility of your big toe is examined, and the capsule and wound are re-approximated with sutures.
4. Lapidus Procedure
The Lapidus is less common. The Lapidus procedure was first described by our division’s founder and is an excellent surgery for those that have moderate to severe bunions in association with a hypermobile joint. This type of procedure may take several months to walk normally after surgery so it is often reserved for severe or extremely degenerative joints.
Repair of the Tendons and Ligaments
The soft tissues around the big toe may be tighter on one side and looser on the other creating an imbalance. This can result in drifting of the big toe towards the second toe. Your surgeon will shorten the loose tissue to tighten it and lengthen the tight tissues to loosen them. This procedure is often combined with an osteotomy.
Arthrodesis
Involves surgical fusion of the damaged bones, followed by insertion of screws, wires, or plates to support the joint while healing. This procedure is used for severe bunions or bunions associated with arthritis. The big toe will have limited movement after the procedure but the bunion will not come back. This type of surgery is rare for bunions.
Benefits of Hallux Valgus Surgery
1. Pain Relief: One of the main reasons people opt to undergo surgery is to relieve the pain that is associated with bunions. Surgery aims to address the misalignment of the toe, which will reduce the discomfort and pain.
2. Improved Functionality: Surgical intervention can greatly improve the functionality of the foot, which will restore a more normal alignment and allow for better weight distribution during activities such as walking or jogging.
3. Expert Surgical Technique: Our team was the first to describe the translational scarf osteotomy, which has demonstrated over a 90% success rate at long-term follow-up. We perform more translational scarf osteotomies than any surgical team in the world.
4. Prevention of Progression: If Bunions are left untreated they tend to become much worse over time. Surgery can prevent the progression of the deformity and the associated symptoms.
5. Correction of Toe Alignment: The surgical procedure will aim to realign the big toe. This will reduce the angle between the first and second toes and in-turn correct the deformity.
6. Enhanced Foot Appearance: For a lot of people, the improvement in terms of aestectics of the foot is a significant benefit. Surgery can address the visible bony bump and result in a more aesthetically pleasing foot appearance for you.
7. Quicker Return to Normal Activities: Depending on the type of surgery, recovery times may vary, but in many cases, patients can return to normal activities with improved foot function after a period of rehabilitation.
8. Increased Comfort in Footwear: After surgery, patients often find it more comfortable to wear a broader range of footwear, as the deformity causing pressure points is corrected.
Risks and Complications of Hallux Valgus Surgery
As with any surgery, complications can occur. Apart from general complications related to all surgeries, complications after bunion surgery can include:
- Infection
- Recurrence of the bunion
- Nerve damage
- Unresolved pain
- The above complications occur in less than 2% of cases
In rare cases, a second surgery may be necessary to correct the problems.