Foot and Ankle Arthritis
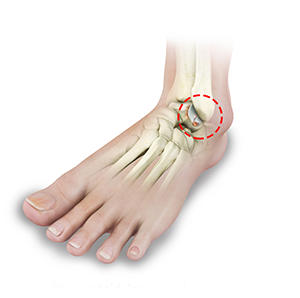
What Ankle Arthritis?
Arthritis is the inflammation of joints as a result of degeneration of the smooth cartilage that lines the ends of bones in a joint. This degeneration of the cartilages leads to painful rubbing of the bones, swelling, and stiffness in the joints, resulting in restricted movements. Arthritis in and the ankle is typically as a result of a previous trauma.
Symptoms of Ankle Arthritis
Pain and swelling around the ankle joint. Restriction in motion, start-up pain
Diagnosis
Clinical diagnosis is made initially through physical examination and supplemented with Xrays, MRI or CT scan.
Treatment
Conservative management consisting of activity modification.
- AFO or lace up ankle foot orthotic, NSAIDS, and occasional steroid injection.
- Biologic augment:
- HA injections (Synvisc)
- PRP growth factors
- Fat stem cells
There are two main types of arthritis that can affect the foot and ankle:
Rheumatoid arthritis: This is an auto-immune disease in which the body’s immune system (the body’s way of fighting infection) attacks healthy joints, tissues, and organs. It can cause pain, stiffness, swelling, and loss of function in the joints. Rheumatoid arthritis mostly affects the joints of the hands and feet and tends to be symmetrical. This means the disease affects the same joints on both sides of the body (both feet) with the same symptoms.
Outcome after single technique ankle arthrodesis in patients with rheumatoid arthritis
Post-traumatic arthritis: Arthritis that develops following an ankle or foot injury is called post-traumatic arthritis. The condition may develop within a short tie or years after the trauma such as a fracture, severe sprain or ligament tears.
What are the Symptoms of Foot and Ankle Arthritis?
The symptoms of foot and ankle arthritis include pain or tenderness, swelling, stiffness in the joint and limited range of motion.
How is Foot and Ankle Arthritis Diagnosed?
The diagnosis of foot and ankle arthritis is made with a medical history, physical examination and X-rays of the affected joint. A bone scan, computed tomography (CT) scans, and magnetic resonance imaging (MRI) scans are also performed to diagnose arthritis.
What are the Treatment Options for Foot and Ankle Arthritis?
Non-surgical treatment options for foot and ankle arthritis include:
- Medications (anti-inflammatories)
- Injections (steroids to reduce inflammation)
- Physical therapy
- Ankle-foot orthosis (AFO)
- Weight loss
- Orthotics such as pads or arch supports
- HA injections (Synvisc)
- PRP growth factors
- Fat stem cells
Surgery may be required to treat foot and ankle arthritis if your symptoms do not improve with conservative treatments. They may include:
- Nano-arthroscopy surgery: The newest form of arthroscopy, otherwise known as ‘needle arthroscopy’ can be performed in office. This utilizes a scope less than 2mm in diameter to visualize joint damage and nano instruments to perform a routine procedure under local anesthesia. The advantage is that the procedure has minimal soft tissue damage and facilitates and early return to function.
- Arthroscopic surgery: Arthroscopy is a surgical procedure during which an arthroscope – a narrow lighted fiber-optic tube with a camera attached – is inserted into the joint through a key-hole incision. The arthroscope provides your surgeon with a large real-time image of the injury on a monitor for a clear view. The internal structures of the joint are examined for diagnosis and your surgeon can treat the problem as well with small surgical instruments passed through 2 – 3 small incisions. Your surgeon uses probes, forceps, knives, and shavers to clean the joint area of foreign tissue, inflamed tissue or bony outgrowths (spurs). Once the surgery is complete, the incisions are closed.
- Joint Arthrodesis: End stage post-traumatic osteoarthrisis (PTOA) or rheumatoid arthritis (RA) may require fusion of the tibiotalar joint. Newer arthroscopic methods of fusion utilizing biologics have accelerated return to function.
- Arthroplasty or joint replacement: In this procedure, your surgeon removes the damaged joint and replaces it with an artificial implant. It is usually performed when the joint is severely damaged by osteoarthritis, rheumatoid arthritis or post-traumatic arthritis. The goal of joint replacement is to relieve pain and restore its normal function.
Dr. Kennedy's Articles
James W, et al. AANA Advanced Arthroscopic Surgical Techniques. The Foot and Ankle. Thorofare, Nj, Slack Incorporated, 2016. Chapter 15: Anatomic Arthroscopic Ankle Arthrodesis