Achilles Tendinitis or Tendinosis
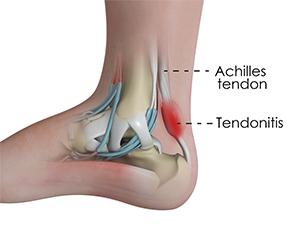
What is Achilles Tendinitis?
Achilles tendinitis is the inflammation and irritation to the Achilles tendon, and occasionally the Achilles tendon sheath. The Achilles tendon is one of the strongest tendons in the body and is responsible for propelling us forward every step we take. Certain activities can cause an overuse injury to the Achilles tendon, particularly in long distance runners and athletes who play sports that utilize sudden deceleration including tennis and squash
Causes of Achilles Tendinitis
Achilles tendinitis occurs as a result of repetitive stress to the tendon. The stress may be due to:
- Overuse of the tendon
- Degeneration of the tendon
- Intense physical activity
- A sudden increase in activity
- Tight calf muscles
- Bone spurs or extra bone growth
Types of Achilles Tendinitis
Based on which part of the tendon is affected, Achilles tendinitis can be differentiated into:
- Insertional Achilles tendinitis: In this type, the lower portion of the tendon, where it attaches (inserts) to the heel bone is inflamed due to bone spurs.
- Non-insertional Achilles tendinitis: In this type, the middle portion of the tendon breaks down with tiny tears (degenerate), swells, and thickens. This is more commonly seen in younger and active people.
Signs and Symptoms of Achilles Tendinitis
Some of the signs and symptoms of Achilles tendinitis include:
- Stiffness and pain along the Achilles tendon.
- Swelling and thickening of the tendon.
- Swelling or discomfort in the back of your heel.
- Pain in the back of your heel that worsens with activity.
- Tight and stiff calf muscle.
- The skin on the heel is warm to touch.
- Limited motion when you flex the foot.
What if Achilles Tendinitis is Left Untreated?
If Achilles tendinitis is left untreated, it may cause:
- Severe pain
- Trouble walking or exercising
- Deformation of the tendon or heel bone
- Total tear or rupture of the Achilles tendon
Risk Factors
The common risk factors that may cause Achilles tendinitis include:
- Sports and Exercise
- Insufficient warming up before exercise
- Poorly-fitting footwear while running
- Running on uneven surfaces or uphill
- Quickly changing your speed
- Sports such as football, baseball, volleyball and tennis
- Certain medication
- Glucocorticoids
- Fluoroquinolones
Symptoms
You may see a swelling at the point of maximal tenderness along the Achilles. The common symptoms of Achilles tendinitis include:
- Morning pain and stiffness along the Achilles tendon
- Severe pain while running, climbing, etc. which occurs initially but then reduces over time during that activity
- Severe pain after activity
- Thickening and fusiform swelling of the tendon
- Inflammation at the back of your heel
- Inability to rise on your toes
Treatment
Inflammation of the Achilles tendon is difficult to treat especially when in an athlete. Traditional treatment requiring periods of long rest is no longer acceptable. We have pioneered many non-operative procedures including shockwave therapy, biologic growth factors and stem cell injections as well as other cutting-edge technologies that can help get patients back into daily activity pain free quickly. For those that require surgery it is rare now to need tendon transfer. Nano arthroscopy in the office has revolutionized treatment and provides immediate benefit under local anaesthetic and most patients get back to sports within two weeks.
Non-Surgical Treatment:
- Exercise: Physical therapy exercises will be taught to enhance your flexibility, range of motion and strength. Functional isometric exercises and eccentric physical therapy is the best in this case.
- Injection therapy:
Platelet Rich Plasma: done in office, this procedure included drawing your blood and spinning it down (centrifuge) until platelets are separated from red blood cells. Platelets have growth factors responsible for regeneration and repair of tendons. These are injected into the Achilles tendon to accelerate healing and relieve inflammation
- Shockwave therapy: Using sound wave treatment once a week for three weeks; pain, inflammation, and swelling may all be reduced.
In office Nano Achilles Tendoscopy
Using a tiny 2mm needle with a high resolution camera attached to the tip, Nano tendoscopy, allows the surgeon to debride the Achilles tendon and treat any small tears in the office setting. This is done while the patient is awake in the office, under a local anaesthetic. Most patients are able to walk the day of surgery and run within a month of the procedure.
Surgical Treatments in the Operating Room:
The standard approach will always start with the in-office Nano tendoscopy. In the case that larger tears are found during this procedure, that are not initially seen on MRI, Dr. Kennedy may choose to convert to a standard OR case requiring a formal repair with debridement. Biologics are used in conjunction, from the patient’s hip, to augment the healing.
Articles/Publications from Dr. Kennedy
- A single platelet-rich plasma injection for chronic midsubstance achilles tendinopathy: a retrospective preliminary analysis
- Extra-corporeal pulsed-activated therapy ("EPAT" sound wave) for Achilles tendinopathy: a prospective study